The association between knee joint biomechanics and neuromuscular control and moderate knee osteoarthritis radiographic and pain severity.
Astephen Wilson JL, Deluzio KJ, Dunbar MJ, Caldwell GE, Hubley-Kozey CL. Osteoarthritis and Cartilage 2010;19:186-193
 It is well-known that radiographic severity of knee osteoarthritis is not strongly related to symptomatic presentation of the disease. In other words, the amount of cartilage deterioration is not associated with the magnitude of functional impairments or pain levels. To help understand what factors are related to structural changes in the knee joint and what factors are related to pain experienced by persons with osteoarthritis, the authors evaluated a set of biomechanical and neuromuscular variables in 40 patients with moderate knee osteoarthritis. The authors used a statistical technique known as Principal Component Analysis to examine the relationship between the predictor variables (knee joint moments, knee flexion angles, walking speed, electromyographic activity from lower extremity muscles and anthropometric/demographic data) and knee joint pain and structural changes in the knee separately. The most interesting finding in this paper was that different factors predict joint pain and structural changes. A greater knee adduction moment, which is a surrogate biomechanical variable of medial knee compartment joint loading, and lower knee flexion angles during gait were predictive of greater radiographic joint severity (r2 = 0.21 and 0.11, respectively). Lower gait speed, lower gastrocnemius activation and greater hamstring muscle activation were associated with more knee pain (r2 = 0.28, 0.16 and 0.10, respectively). Multiple linear regressions revealed that a combination of greater knee adduction moment and greater body mass index was associated with greater radiographic disease severity.
It is well-known that radiographic severity of knee osteoarthritis is not strongly related to symptomatic presentation of the disease. In other words, the amount of cartilage deterioration is not associated with the magnitude of functional impairments or pain levels. To help understand what factors are related to structural changes in the knee joint and what factors are related to pain experienced by persons with osteoarthritis, the authors evaluated a set of biomechanical and neuromuscular variables in 40 patients with moderate knee osteoarthritis. The authors used a statistical technique known as Principal Component Analysis to examine the relationship between the predictor variables (knee joint moments, knee flexion angles, walking speed, electromyographic activity from lower extremity muscles and anthropometric/demographic data) and knee joint pain and structural changes in the knee separately. The most interesting finding in this paper was that different factors predict joint pain and structural changes. A greater knee adduction moment, which is a surrogate biomechanical variable of medial knee compartment joint loading, and lower knee flexion angles during gait were predictive of greater radiographic joint severity (r2 = 0.21 and 0.11, respectively). Lower gait speed, lower gastrocnemius activation and greater hamstring muscle activation were associated with more knee pain (r2 = 0.28, 0.16 and 0.10, respectively). Multiple linear regressions revealed that a combination of greater knee adduction moment and greater body mass index was associated with greater radiographic disease severity.This study highlights an important aspect of osteoarthritis: although the severity of osteoarthritis is frequently graded using radiographs, clinical decisions related to treatment of the disease come as a result of both symptomatic presentation AND structural changes within the joint. An orthopaedic surgeon would never perform a total knee arthroplasty on a patient with radiographic evidence of knee OA, but who had no pain. This paper adds evidence to the fact that structural changes may be the result (or consequence) of biomechanical alterations, but pain drives changes in muscle control patterns and gait speed. The biomechanical variables that were predictive of structural changes are not a novel finding; the knee adduction moment is strongly related to disease progression and each pound of weight gained results in a four-fold increase in joint compression forces. However, it does suggest that if we want to affect the structural changes associated with the disease, we should encourage patients to lose weight and to use a device to reduce the adduction moment (either bracing or gait retraining). It also suggests that in order to improve gait speed and decrease abnormal hamstring activity, we need to modify pain. Future longitudinal and interventional studies are needed to support these conclusions, but these findings suggest that pain and disease severity need to be considered when interpreting biomechanical and neuromuscular changes in persons with knee osteoarthritis.
Written by: Joseph Zeni, Jr
Reviewed by: Stephen Thomas

Joe great post. Since the study only looked at one visit, it seems that we can't definitively state what's causing what but rather that these things are related. From a clinical point of view, do you think it would be reasonable to flip around the pain findings and say that a person experiencing knee pain may have a slower walking speed and altered muscle activation? Therefore, as clinicians we should be careful with how we manage/advise patients (especially active patients) that are experiencing knee pain?
Have you seen any clinical trials testing the influence of knee braces that reduce adduction moments (e.g., unloader braces) on structural change over time? How effective are these braces at altering the mechanics (let alone the fact that many patients I have seen will eventually walk in wearing them wrong)?
Thanks!
Jeff – from this study alone we can't assume causation in either direction. That being said, we do know that the adduction moment is the best predictor if disease progression in long term follow-up. with greater adduction moment related to greater progression of the disease. In fact a relatively small increase in the adduction moment (typically about 1/4 of the within subject average), results in a 6 times increase in the chance for disease progression. (For a full review of this article see Miyazaki et al. Dynamic load at baseline can predict radiographic disease progression in medial compartment knee osteoarthritis from Ann Rheum Dis 2002;61:617–622 – https://ard.bmj.com/content/61/7/617.abstract.)
There are conflicting reports about the efficacy of bracing to reduce the load and what the clinical implications of using the brace are. The general consensus is that the braces can reduce the adduction moment, but how practical they are (given patient compliance issuues, expense, burden of wearing a brace with dress clothes, etc,) is the subject of a hot clinical debate. It would be interesting to get the clinicians perspective if anyone has experience using them for their patients. There are also other promising areas to reduce the adduction moment, including lateral shoe wedges, which may be the least invasive and most practical method of reducing this moment. Some long term studies have shown good success with these devices. Other potential clinical interventions include gait retraining (see Barrios et al. for more information – https://linkinghub.elsevier.com/retrieve/pii/S0021929010002022) or more invasive procedures including tibial osteotomies. Future, longitudinal studies are needed for all of these interventions to truly determine their long-term efficacy at improving function and reducing the risk of disease progression.
Hello!
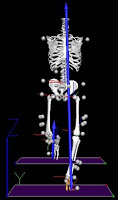
I wonder how have you drawn the ground reaction force vectors without constructing force vectors of gravity impacting on the body, then transmitted through the necks of the femurs and down to the feet? Your figure seems to contradict the laws of Physics if not PROVEN otherwise but it doesn't look going hand in hand with those laws.
Dr. Vladimir Petrunko