Longitudinal Assessment of Depressive Symptoms After Sport-Related Concussion in a Cohort of High School Athletes
Hammer E, Hetzel S, Pfaller A, McGuine T. Sports Health. 2020 Aug 28;1941738120938010
https://pubmed.ncbi.nlm.nih.gov/32857687/
Take-Home Message
High school athletes with a concussion report depression symptoms up to 7 days after an injury; however, these emotional symptoms may resolve over 12 months.
Summary
There are conflicting reports that people with a history of a concussion may be more likely to experience depression (see related posts below). These conflicting findings are hard to interpret because the original authors were unable to follow people for months or years, starting at or before the time of injury. It is important to illustrate the long-term effects following a concussion to promote improved prevention and management strategies. Therefore, the authors performed a prospective cohort study of 2160 high school athletes to assess the depression symptoms over a year after a concussion. The authors recruited athletes from 31 urban, suburban, and rural Wisconsin high schools from August 2016 to November 2018. Before the student-athlete’s sport season they completed the Patient Health Questionnaire-9 (PHQ-9), a screening tool for 9 depressive symptoms (points range from 0-27). Higher scores (>5) indicate signs of depression. Additionally, student-athletes completed the SCAT5 sign and symptom checklist, where they rate each of the symptoms on a 7-point Likert scale. When an athlete sustained a concussion, they were reevaluated within 24-72 hours, 7 days, time of return to play, 3 months, 6 months, and 12 months.
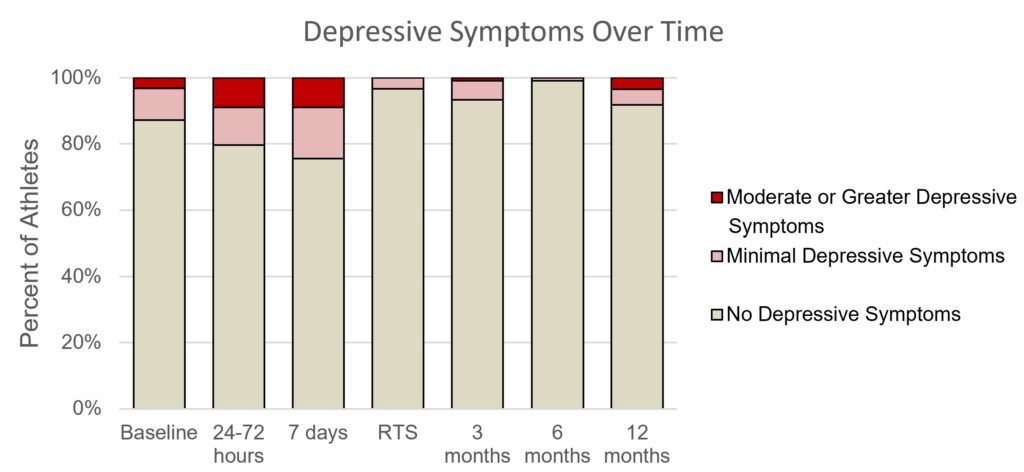
A total of 125 student-athletes (36% female; ~16 years of age) suffered a sport-related concussion, where 29% had a history of concussion. Football was the most common sport for male concussions (78%). Volleyball (31%), basketball (24%), and soccer (20%) were the most common sports for female’s concussions. Fifty-eight percent of the student-athletes returned to play within 14 days, and 92% of the cohort returned within 28 days. Compared with baseline test scores, depression symptoms worsened by ~1 point at both 24-72 hours and 7-day time points. However, depressive symptom scores improved compared to baseline scores at return to play, 3 months, and 6 months after an injury. While the average differences are small, the figure highlights that slightly more student-athletes may report depressive symptoms during the first week after a concussion.
Viewpoints
The researchers found that high school athletes reported more depressive symptoms acutely following a sport-related concussion, and the reported symptoms improved by their return to play. More research should be done in this area because students may report feeling better to return to play. Furthermore, on average, the authors detected small changes (~1 point) in depressive symptoms, which may not be clinically meaningful. However, the authors demonstrated that almost 1 in 8 athletes reported depressive symptoms at baseline and then almost twice as many student-athletes reported depressive symptoms 7 seven days after a concussion. Screening for depressive symptoms at baseline and after a concussion could help identify students that would benefit from additional care. It should be noted that only 68% of the participants completed the 12-month visit. Since it is possible athletes could have dropped out due to depressive symptoms, larger studies may be needed to see who is likely to drop out and to assess the long-term prognosis after a concussion. Currently, medical professionals should be aware of the common depressive symptoms that student-athletes can experience after a concussion. Further, medical professionals should consider patient-reported outcome measures – such as the PHQ-9 – to identify athletes at risk of depression at baseline and/or after an injury. This could lead to mental health evaluations/consultations to ensure an athlete’s wellness.
Questions for Discussion
What is your experience with assessing quality of life and depression following a concussion? Do you implement these measures at baseline? If not, do you feel it is necessary and/or worthwhile to document and track following an injury?
Written by: Jane McDevitt
Reviewed by: Jeffrey Driban
Related Posts
Playing High School Football May Not Lead to Impaired Cognition of Depression
Concussions and Depression…Is there a Connection?
Baseline Neurocognitive Performance and Symptoms May be Influenced by Depression


